The UD researchers have devised tiny cargo-carrying systems many times smaller than a human hair. These systems, or carriers, are made from molecules called peptides that help provide structure for cells and tissues.
The research team is working to program these nanoparticle carriers to selectively bind to degrading collagen in the body. Collagen is a protein that helps plump up or provide structure to connective tissue—everything from our skin to our bones, tendons and ligaments.
When collagen degrades, as a result of disease or injury, the nanoparticles designed by the Kiick lab can attach and remain at the injury site longer than many current treatment options. This allows for the possibility of delivering site-specific medicines over longer periods of time—from days to weeks.
In one collaborative project that involves this work, Kiick is trying to develop drug carriers that could be useful in treating osteoarthritis. Osteoarthritis is a degenerative joint disorder characterized by inflammation, pain and stiffness. According to the Centers for Disease Control and Prevention, it affects 32.5 million Americans.
Early studies with Christopher Price, an associate professor in biomedical engineering, suggests that these nanoparticles can be retained in tissue and knee joints. In other related studies, Kiick and her students have shown that drugs can be encapsulated and retained in the nanoparticles, until released by changes in temperature.
“We are interested in learning how to release drugs that can help not just with pain management, but also with slowing down disease progression,” said Kiick, Blue and Gold Distinguished Professor of Materials Science and Engineering. “It has been key that we have been able to collaborate with the Price laboratory in this type of work.”
For a long time, small molecule corticosteroids have been a standard of care for managing pain in osteoarthritic joints. Because the joint is full of thick, sticky fluid and is under constant mechanical stress and motion, these small-molecule drugs get expelled from the fluid around the knee pretty quickly, in minutes.
“We are hopeful that by controlling the nanoparticle composition and structure,” said Kiick, “we will be able to finely control, or tune, the drug delivery behavior to provide longer-lasting relief for people with inflammatory conditions, such as osteoarthritis.”
Kiick and colleagues reported advances on the nanoparticle design on Wednesday, Oct. 7, in a paper published in Science Advances, a peer-reviewed journal of the American Association for the Advancement of Science. Co-authors on the work include Jingya Qia, a graduate student in the Kiick lab, and Jennifer Sloppy, a senior microscopy specialist in UD’s Harker Interdisciplinary Science and Engineering Laboratory.
The paper’s key findings demonstrate the research team’s ability to control the shape of the nanoparticles, which will impact how well they can bind to tissue in the body and stay in a particular location. The research team also can precisely control the size of the nanoparticles, which has implications for how they might be retained at the injection site and also how they may be used by particular cells before being removed from the body. Finally, the paper describes some of the very fine details of how the specific building blocks inside these peptide molecules can affect the temperature at which those different shaped and sized nanoparticles can be disassembled to release a medicine.
The research builds on Kiick’s previous patented and patent-pending work in this area, but she said it is collaboration with others that is driving forward promising results. While the Kiick lab brings expertise in creating novel materials that can be used as delivery systems; Arthi Jayaraman, Centennial Term Professor for Excellence in Research and Education in the Department of Chemical and Biomolecular Engineering, is helping the team understand factors related to temperature sensitivity of the delivery vehicles and to develop computational tools that can help the research team characterize the vehicle’s shape.
Meanwhile, Price’s expertise in understanding post-traumatic osteoarthritis has been key to developing methods to use these nanoparticles to potentially treat disease. Price is exploring how particular drugs and cells interact, which may inform what specific classes of medicines are useful in treating osteoarthritis that develops following traumatic injury. The collaboration will help the Kiick lab tailor what types of nanoparticle devices can be used to deliver these different classes of medicines.
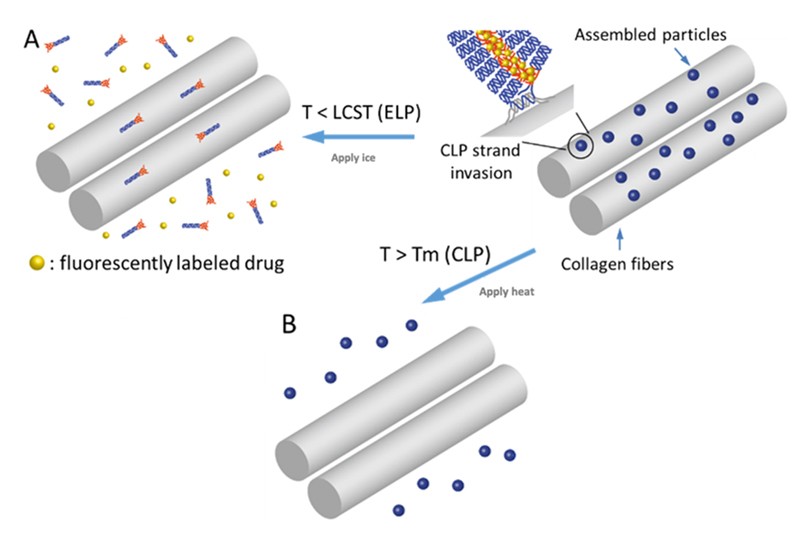
According to Kiick, thinking big, the team could imagine loading a custom cocktail of medicines into the drug-delivering nanoparticles capable of delivering relief over varying timescales and temperatures. The researchers already have the right material nanostructure that can allow this to happen; now they are exploring how to trigger the nanoparticles to release specific medications under particular conditions.
“You could imagine injecting these encapsulated medications at the knee,” she explained. “Then, when you want one medication to be released, the patient could ice their knee. If another drug is needed to provide relief over a longer time-period, heat could be applied.”
It could be a really simple way to help people manage chronic conditions that cause a lot of pain and reduce mobility. And because the treatment is local, it could reduce side effects that can occur when drugs have to be taken at high doses or over prolonged periods of time.
“If these delivery vehicles could reduce painful effects of osteoarthritis, or delay when osteoarthritis symptoms emerge, there could be important implications for improving quality of life for many people,” Kiick said.
Read the original article on University of Delaware.