Drugs and vaccines circulate through our vascular system reacting according to their chemical and structural nature. In some cases, their destination is diffuse. In other cases, like cancer treatments, the intended target is highly localized. The effectiveness of a medicine —and how much is needed and the amount of side-effects it causes —are a function of how well it can reach its target.
"A lot of medicines involve intravenous injections of drug carriers," said Ying Li, an assistant professor of Mechanical Engineering at the University of Connecticut. "We want them to be able to circulate and find the right place at the right time and to release the right amount of drugs to safely protect us. If you make mistakes, there can be terrible size-effects."
Li studies nanomedicines and how they can be designed to work more efficiently. Nanomedicine involves the use of nanoscale materials, such as biocompatible nanoparticles and nanorobots, for diagnosis, delivery, sensing or actuation purposes in a living organism. His work harnesses the power of supercomputers to simulate the dynamics of nanodrugs in our blood stream, design new forms of nanoparticles, and find ways to control them.
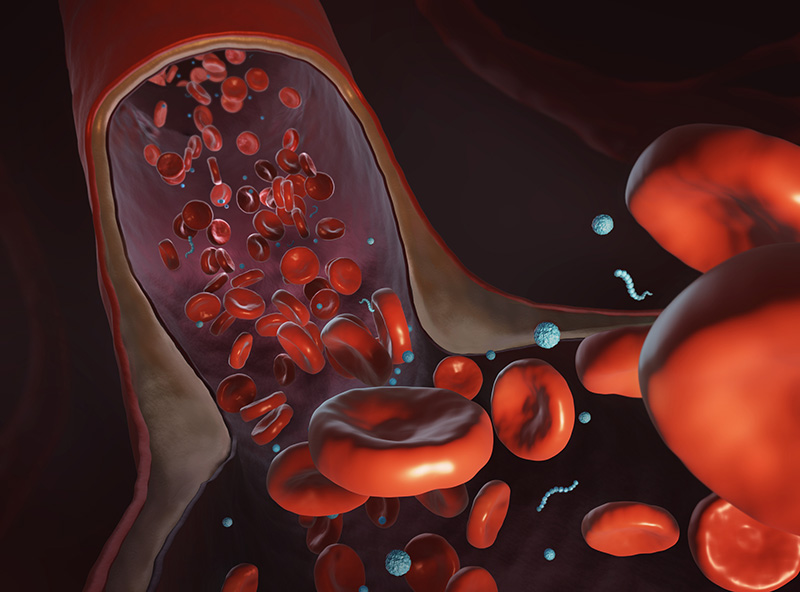
Red blood cell hitchhiking enhances the accumulation of nano- and micro-particles in the constriction of a stenosed microvessel.
Over the last decade, with support from the National Science Foundation, Li and his team have investigated many key aspects of nanomedicines, pioneering methods to model their flow and how they interact with structures within the body.
"My research is centered on how to build high-fidelity, high-performance computing platforms to understand the complicated behaviors of these materials and the biological systems down to the nanoscale," he said.
"I'm a 100% computational person, there's no dirty hands," Li joked. "Because of the size of these particles, this problem is very hard to study using experiments."
Writing in Soft Matter in January 2021, Li described the results of a study that looked at how nanoparticles of various sizes and shapes —including nanoworms — move in blood vessels of different geometries mimicking the constricted microvasculature. Nanoworms are long, thin, engineered encapsulations of drug contents.
"We found that the transport of these nanoworms is dominated by red blood cells," which make up 40% to 50% of the flow, Li explained. "It's like driving on the highway — construction slows down traffic. Drugs are getting carried by individual red blood cells and dragged into narrow regions and getting stuck."
He determined that nanoworms can travel more efficiently through the bloodstream, passing through blockages where spherical or flat shapes get stuck.
"The nanoworm moves like a snake. It can swim between red blood cells making it easier to escape tight spots," Li said.
Speed is of the essence — drugs must reach their destination before they are discovered and neutralized by the body's immune system, which is always on the hunt for foreign particles.
The first nanoparticle-based treatment to be FDA approved for cancer was Doxil — a formulation of the chemotherapy agent doxorubicin. Many more are currently in development. However, a 2016 study in Nature Material Review found only 0.7% of an administered nanoparticle dose is delivered to a solid tumor.
"We know that anti-cancer drug molecules are highly toxic," Li said. "If they don't go to the right place, they hurt a lot. We can reduce the dosage if we actively guide the delivery."
Tailor-made shapes are one way to improve the delivery of cancer drugs. (Currently 90% of administered nanoparticles are spherical.) Another way is to coax drugs to their target.
Li's team has computationally modeled nanoparticles that can be manipulated with a magnetic field. In a 2018 paper in the Proceedings of the Royal Society, they showed that even a small amount of magnetic force could nudge the nanoparticles out of the blood flow, leading to a far greater number of particles reaching the right destination.
Li's work is powered by the Frontera supercomputer at the Texas Advanced Computing Center (TACC), the ninth fastest in the world. Li was an early user of the system when it launched in 2019, and has used Frontera continuously since then to perform a variety of simulations.
"We're building high-fidelity computational models on Frontera to understand the transport behavior of nanoparticles and nanoworms to see how they circulate in blood flow," Li said. His largest models are more than 1,000 micrometers long and include thousands of red blood cells, totaling billions of independent ways that the system can move.
"Advanced cyberinfrastructure resources, such as Frontera, enable researchers to experiment with novel frameworks and build innovative models that, in this example, help us understand the human circulatory system in a new way," said Manish Parashar, Director of the NSF Office for Advanced Cyberinfrastructure. "NSF supports Frontera as part of a broader ecosystem of cyberinfrastructure investments, including software and data analytics, that push the boundaries of science to yield insights with immediate application in our lives."
Frontera allows Li not only to run computational experiments, but also to develop a new computational framework that combines fluid dynamics and molecular dynamics.
Writing in Computer Physics Communications in 2020, he described OpenFSI: a highly efficient and portable fluid–structure simulation package based on the immersed-boundary method. The computational platform serves as a tool for the broader drug-design community and can be translated for many other engineering applications, such as additive manufacturing, chemical processing, and underwater robotics.
"The current computational model covers many important processes, but the whole process is so complicated. If you consider a patient-specific vasculature network, that makes our computational model intractable," Li said.
He is taking advantage of artificial intelligence (AI) and machine learning to serve as a high-speed vehicle for the rapid generation of new nanoparticle designs and methods. Like all AI and machine learning, this approach requires massive quantities of data. In Li's case, the data is coming from simulations on Frontera.
"We're currently building the training database for the machine learning aspect of our work. We ran a lot of simulations with different scenarios to get broad training data," Li explained. "Then, we can pre-train the neural network using the hypothetical data we take from these simulations so they can quickly and efficiently predict the effects."
Li's typical simulations use 500 to 600 processors, though some aspects of the research requires up to 9,000 processors computing in parallel. "My research productivity is correlated with the speed of the system I use. Frontera has been fantastic."
When people picture medical research, they typically think of lab experiments or drug trials, but there are limitations to this type of work, whether economic or physical, Li said.
"The computational approach is getting more powerful and more predictive," he said. "We should take advantage of computational simulations before we run very expensive experiments to rationalize the problem and provide better guidance."
Read the original article on Texas Advanced Computing Center.