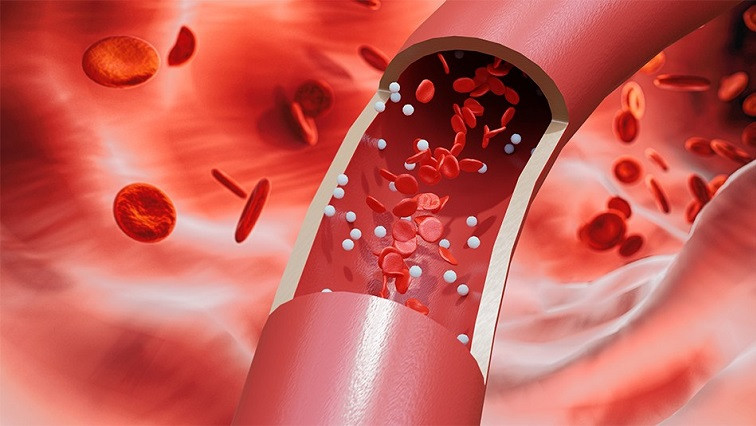
Vascular diseases like atherosclerosis can lead to serious complications, like heart attack or stroke. But many treatments for these diseases target systemic risk factors, such as reducing blood pressure and cholesterol, rather than repairing damaged blood vessels themselves.
A new targeted nanomedicine treatment developed at the University of Chicago has shown promise in reducing vascular lesions caused by atherosclerosis in a mouse model.
The research, a collaboration between Matthew Tirrell, dean of the Pritzker School of Molecular Engineering, and Yun Fang, professor of medicine in the Biological Sciences Division, could ultimately lead to better treatments for humans who suffer from complications of vascular disease.
The results were published in the Proceedings of the National Academy of Sciences.
“We are really enthusiastic about this technology,” Tirrell said. “It directly targets the site of the inflammation and could have implications in a variety of vascular disorders.”
Delivering medicine directly to inflamed cells
In vascular diseases like atherosclerosis, arterial walls thicken and harden, disturbing blood flow. That leads to a buildup of plaque, which could ultimately lead to blocked arteries.
Studies have linked microRNA-92a (miR-92a) to dysfunction of the endothelial cells that line the inside of blood vessels, which means miR-92a is considered a biomarker of the disease.
While an miR-92a inhibitor treatment exists (and has been tested in animals and humans), it cannot yet be delivered directly to the blood vessel site, and therefore is not as effective as it could be. Several years ago, Tirrell and Fang developed a nanoparticle — a polyelectrolyte complex micelle — to deliver the inhibitor directly to inflamed blood vessel cells.
This nanoparticle uses a peptide to target the vascular cell adhesion molecule 1 (VCAM-1), which is found in high levels in inflamed endothelial cells but remains low in healthy cells. Once the peptide finds the molecule, it delivers the miR-92a inhibitor directly to the damaged cells.
A new tool to improve outcome of stent insertions
The team has tested the nanomedicine in a mouse model and found that it reduces the size of vascular lesions. They also found that the treatment inhibited stenosis, the remodeling of vascular tissue that causes it to close off.
“That means this nanoparticle could be used during treatments like angioplasty or the insertion of a stent, improving outcomes of those procedures and reducing the chance of stenosis,” Tirrell said. It could also be used to treat patients who are suffering from complications of vascular disease. This is especially important, since many patients who have a cardiovascular event, like a heart attack, often have a secondary event afterward.
“Our nanoparticle could be used to prevent subsequent cardiovascular events,” Fang said.
The team will continue to test the treatment with the goal of eventually completing human trials.
“Almost all vascular disorders are associated with this inflammation, so this treatment could be used toward a wide range of diseases,” Fang said.
Read the original article on University of Chicago.