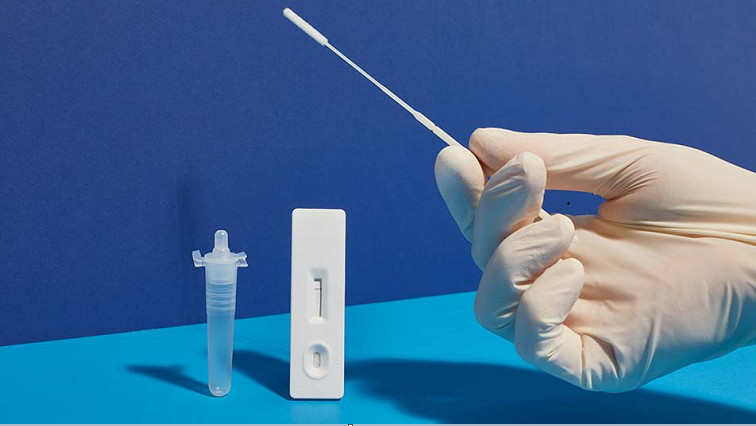
Rapid antigen tests can quickly and conveniently tell a person that they are positive for Covid-19. However, because the antibody-based tests aren’t very sensitive, they can fail to detect early infections with low viral loads.
Now, a research team led by Newcastle University experts, reporting in ACS Sensors, has developed a rapid test that relies on molecularly imprinted polymer nanoparticles, rather than antibodies, for detection.
The team involves researchers at Newcastle University, comprised of Jake McClements, Pankaj Singla, Marloes Peeters, Shayan Seyedin and Brendan Payne, who worked with MIPDiagnostics, Manchester Metropolitan University and Université Libre de Bruxelles.

A 3D-printed device detects thermal resistance changes when SARS-CoV-2 binds to molecularly imprinted polymer nanoparticles.
Advantages of the new test
Lead author, Dr Marloes Peeters, Senior Lecturer at Newcastle University’s School of Engineering, said: “We develop a new type of Covid-19 test which has many advantages over current lateral flow tests. For example, lateral flow tests use biological antibodies to trap and detect the Covid-19 virus, whereas we use a synthetic alternative known as polymer antibodies. This allows for a test which is as fast - 15 mins, and cheap as a lateral flow test but can detect 6000-times smaller amounts of the Covid-19 virus. Consequently, this will improve test accuracy, particularly for asymptomatic or pre-symptomatic individuals. Moreover, synthetic antibodies are very robust which means the tests have a longer shelf-life, can be used in hot climates with no issues and will not produce false-positive results in acidic media, such as soft drinks.
“In the future, we hope to further validate our polymer antibody by testing more patient samples, including saliva samples and samples from the omicron variant. Additionally, the polymer antibodies can be easily adapted for any new Covid-19 variants or other emerging pathogens.”
The gold standard for Covid-19 diagnosis remains the reverse transcription-polymerase chain reaction (RT-PCR). Although this test is highly sensitive and specific, it takes 1-2 days to get a result, is expensive and requires special lab equipment and trained personnel. In contrast, rapid antigen tests are fast (15-30 minutes), and people can take them at home with no training, but they lack sensitivity, sometimes resulting in false negatives. Also, the tests use antibodies against SARS-CoV-2 for detection, which can’t withstand wide ranges of temperature and pH. The research team colleagues wanted to make a low-cost, rapid, robust and highly sensitive Covid-19 test that uses molecularly imprinted polymer nanoparticles (nanoMIPs) instead of antibodies.
To make nanoMIPs, the researchers began by attaching a peptide from the SARS-CoV-2 spike protein to a solid support. Then, they added nanoparticle building blocks and polymerized them around the peptide, creating nanoparticles with a binding site specific for the coronavirus spike protein. They isolated the nanoparticles that bound most strongly to the peptide and attached them to a screen-printed electrode. After showing that the nanoMIPs could bind SARS-CoV-2, they added the electrode to a small 3D-printed device that measured changes in thermal resistance that occurred upon binding.
When the team added samples from seven patient nasopharyngeal swabs to the device, the liquid flowed over the electrode, and the researchers detected a change in thermal resistance for samples that had previously tested positive for Covid-19 by RT-PCR. The test required only 15 minutes, and preliminary results indicated that it could detect a 6,000-times lower amount of SARS-CoV-2 than a commercial rapid antigen test. Unlike antibodies, the nanoMIPs withstood warm temperatures — which could give the test a longer shelf life in hot climates — and acidic pH — which might make it useful for monitoring SARS-CoV-2 in wastewater. However, to prove that the test has a lower false negative rate than existing rapid antigen tests, it must be tested on many more patient samples, the researchers say.
Read the original article on Newcastle University.