Sepsis, the body’s overreaction to an infection, affects more than 1.5 million people and kills at least 270,000 every year in the U.S. alone. The standard treatment of antibiotics and fluids is not effective for many patients, and those who survive face a higher risk of death.
In new research published in the journal Nature Nanotechnology today, the lab of Shaoqin “Sarah” Gong, a professor with the Wisconsin Institute for Discovery at the University of Wisconsin–Madison, reported a new nanoparticle-based treatment that delivers anti-inflammatory molecules and antibiotics.
The new system saved the lives of mice with an induced version of sepsis meant to serve as a model for human infections, and is a promising proof-of-concept for a potential new therapy, pending additional research.
The new nanoparticles delivered the chemical NAD+ or its reduced form NAD(H), a molecule that has an essential role in the biological processes that generate energy, preserve genetic material and help cells adapt to and overcome stress. While NAD(H) is well known for its anti-inflammatory function, clinical application has been hindered because NAD(H) cannot be taken up by cells directly.
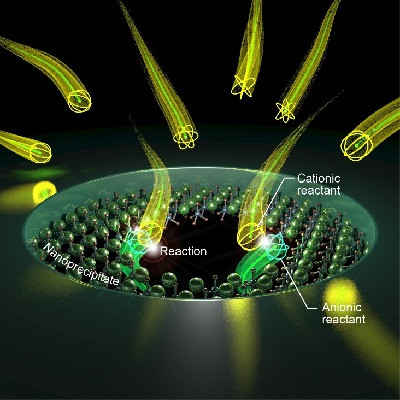
“To enable clinical translation, we need to find a way to efficiently deliver NAD(H) to the targeted organs or cells. To achieve this goal, we designed a couple of nanoparticles that can directly transport and release NAD(H) into the cell, while preventing premature drug release and degradation in the bloodstream,” says Gong, who also holds appointments in the Department of Biomedical Engineering and the UW School of Medicine and Public Health’s Department of Ophthalmology and Visual Sciences.
The interdisciplinary work was led by Gong along with Mingzhou Ye and Yi Zhao, two postdoctoral fellows in the Gong lab. John-Demian Sauer, a professor in the Department of Medical Microbiology and Immunology, also collaborated on the project.
Sepsis can be deadly in two phases. First, an infection begins in the body. The immune system responds by creating drastic inflammation that impairs blood flow and forms blood clots, which can cause tissue death and trigger a chain reaction leading to organ failure. Afterward, the body overcorrects itself by suppressing the immune system, which in turn increases infection susceptibility. Controlling complications caused by inflammation is vital in sepsis therapy.
The lipid-coated calcium phosphate or metal-organic framework nanoparticles designed by the Gong lab can be used to co-deliver NAD(H) and antibiotics. Gong’s lab tested the NAD(H)-loaded nanoparticles in multiple mouse models including endotoxemia, multidrug-resistant pathogen-induced polymicrobial bacteremia, as well as a puncture-induced sepsis model with secondary infection by a common illness-causing bacteria called P. aeruginosa.
The nanoparticle treatment performed much better than using NAD(H) alone. For instance, in an endotoxemia mouse model, mice without any treatment or treated with free NAD(H) died within two days. In contrast, mice treated with NAD(H)-loaded nanoparticles all survived. These animal studies demonstrated that the NAD(H) nanoparticles can help maintain a healthy immune system, support blood vessel function and prevent multiorgan injury.
This technology may pave the road for the development of a new clinical therapy for sepsis that could also be applied in other inflammation-related scenarios, such as COVID-19 treatment. An additional benefit of this therapy is the ability to treat infection with lower amounts of antibiotics, which reduces their overuse. Further research in larger animal models will be necessary before clinical trials in people could begin.
“The NAD(H) nanoparticles have the potential to treat many other diseases because NAD(H) is involved with so many biological pathways. There is strong evidence for the use of NAD(H) as an intervention or aid in critical illnesses,” says Gong.
Read the original article on University of Wisconsin–Madison.