UCF material sciences engineers Melanie Coathup and Sudipta Seal have designed a cerium oxide nanoparticle — an artificial enzyme — that protects bones against damage from radiation. The nanoparticle has also shown abilities to improve bone regeneration, reduce loss of blood cells and help kill cancer cells.
Their study, a collaboration with Oakland University, North Carolina A&T University, the University of Sheffield and University of Huddersfield in the U.K., was published in Bioactive Materials.
Approximately 50% of all cancer patients receive radiation therapy — a treatment that uses electrically charged particles to kill cancer cells. About 40% of patients are cured with this therapy. However, bone damage is a side effect, impacting about 75% of patients receiving radiation.
“Because of its high calcium content, bone absorbs 30-40% more radiation than other tissues and so it is a common site of injury,” says Coathup, director UCF’s Biionix faculty cluster. “Radiation makes the bone brittle and easily fractured. And due to the damage caused by radiation, many people are then unable to repair their bone fracture. In some people, this leads to having an amputation to resolve the complication.”
While radiotherapy beams are directly aimed at the tumor, surrounding healthy tissue also gets damaged and can cause many additional health issues for patients.
“At the moment, there is no real drug or therapy to protect healthy tissue from the damage caused by radiation,” Coathup says. “This is not only a problem for cancer patients who undergo radiotherapy but also poses problems for astronauts and future deep space exploration.”
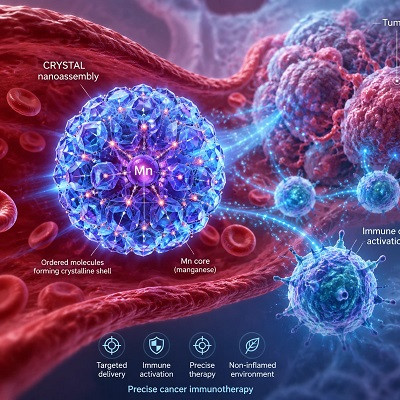
The body’s natural defense against radiation is a group of enzymes called antioxidants — but this defense system gets easily overwhelmed by radiation and on its own cannot protect the body from damage. Seal, a leading nanotechnologist, designed the cerium oxide nanoparticle — or nanoceria — that mimics the activity of these antioxidants and has a stronger defense mechanism in protecting cells against DNA damage.
“The nanoceria works with a specifically designed regenerative lattice structure responsible for destroying harmful reactive oxygen species, a byproduct of radiation treatment,” Seal says.
Working with postdoctoral researcher Fei Wei, Coathup tested the nanozyme in live models receiving radiation therapy.
“Our study showed that exposing rats to radiation at similar levels to those given to cancer patients led to weak and damaged bones,” Coathup says. “However, when we treated the animals with the nanozyme, before and during three doses of radiation over three days, we found that the bone was not damaged, and had a strength similar to healthy bone.”
The study also showed that the nanozyme treatment helped kill cancer cells, possibly due to an increase in acidity, and protected against the loss of white and red blood cells that usually occurs in cancer patients. A low white and red blood cell count means the patient is more susceptible to opportunistic infection, less able to fight cancer and is more fatigued. Another interesting find is that the nanoparticle also enhanced healthy cells’ ability to produce more antioxidants, reduced inflammation (which also leads to bone loss) and promoted bone formation.
Future research will seek to determine appropriate dosage and administration of the nanozyme and further explore how nanozyme helps to kill cancer cells. The researchers will also focus their studies in the context of breast cancer, as women are more susceptible to bone damage than men.
“Cancer patients are already struggling with fighting one disease,” Coathup says. “They shouldn’t have to be worried about bone fractures and tissue damage. So we’re hoping this breakthrough will help survivors go back to living a normal and healthy life.”
Coathup completed her undergraduate studies in medical cell biology and earned a Ph.D. in orthopedic implant fixation at University College London in the U.K. In 2017 she joined the College of Medicine and became the director of UCF’s Biionix faculty cluster — a multidisciplinary team of researchers working to develop innovative materials, processes and interfaces for advanced medical implants, tissue regeneration, prostheses, and other future high-tech products.
Read the original article on University of Central Florida.