A new paper published in the Journal of Controlled Release reports the methodical development of lipid-peptide nanocomplexes as a delivery vehicle for messenger ribonucleic acid (mRNA) molecules to the tumor cell, in vitro and in vivo. The encouraging results warrant more research on these potential anti-tumor immunotherapy vehicles.
Introduction
The range and utility of mRNA are increasing rapidly over time. It is capable of adding or replacing deficient or defective proteins to the cells of a host organism using the physiological mechanisms of the host itself. It can also be used to encode foreign antigens, for instance, the spike protein antigen of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
The advantages of mRNA relative to DNA include its ability to undergo transfection faster than DNA-containing plasmids. This is because the former does not have to be transferred from the nucleus to cytosol via the nuclear membrane, a primary barrier in differentiated cells. Instead, once the mRNA is in the cytosol, it can bind to the ribosomes to translate the code into actual proteins.
Since the mRNA is not incorporated into the chromosomal DNA, the genotoxic effects are much less likely. Moreover, its manufacture is much easier than that of DNA plasmids. The latter are also much larger, about 5-10 kb, with a double-stranded supercoiled structure, compared to the linear single-stranded nature of mRNA.
However, ribonuclease enzymes are found throughout the body, and these degrade mRNA before it can achieve its intended effects. Moreover, the mRNA needs to reach the affected tissue and enter the cells. Being a large molecule with a negative charge, and hence unable to pass across the lipid bilayer membrane, this is achieved via endocytosis.
At the same time, it must not be broken down by the endosomes. To meet these twin challenges, the researchers explored the use of virus-sized nanoparticles containing both lipids and peptides to deliver the mRNA to the cells.
While lipid nanoparticles (LNPs) were used to deliver the SARS-CoV-2 spike antigen to the cells, they need to be optimized for effective mRNA transfection. The current paper looked at the use of hybrid particles that combined lipids with polymers or peptides to make the resulting LNPs more effective at entering the cell and avoiding intra-endosomal destruction.
Findings
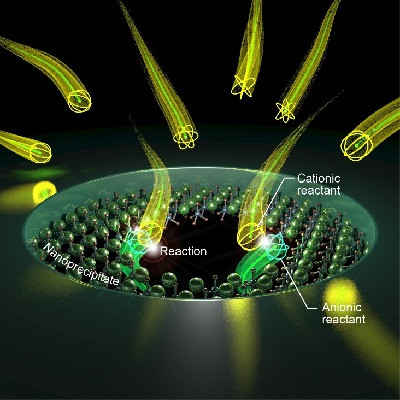
The authors followed a systematic approach to optimize a nanocomplex of lipids and peptides in electrostatic complex with mRNA, and identified some of the unique features that may be helpful in taking these findings further for mRNA-based therapeutic agents.
In previous work, the authors had described the inclusion of a number of different lipids such as DOTMA and DOPE, that promote membrane fusion and thus avoid endosomal catabolism, as well as various peptides. Some peptides have a cationic oligolysine motif that can bind mRNA electrostatically, while others have motifs that target receptors to promote mRNA uptake.
Using a strategy called multifactorial screening, the researchers optimized individual lipids and peptides. Various formulations were then subjected to screening in vitro and in vivo to identify those that worked best.
For one thing, nanocomplexes of lipids and peptides worked best when the peptide was added last in order, probably because of greater peptide exposure in the final nanocomplex, with better receptor targeting and nanocomplex uptake. The ratio of the components for optimal transfection varied between different cell lines.
DOPE and peptide 35 were included in most of the top formulations, and those with RVRR linkers. This suggests that the helper lipid must be chosen carefully, both for its own properties and in combination with the other components of the formulation.
The linker is important in that its cleavage by furin or cathepsin B, within the endosome, cuts the ligand away from the nanocomplex, setting it free from the receptor. This allows it to move into the cytosol.
In fact, the formulation containing C14, DOPE and peptide 35 had an 8-fold greater transfection efficiency than the original formulation, with a small increase in cell viability. When 30% cholesterol was added, a further 5-fold improvement was observed.
Such findings were validated in vivo, using mouse subcutaneous tumors. Further analysis showed this to be due to an increased amount of mRNA within the transfected cells, rather than a higher number of transfected cells.
Furthermore, cholesterol increased the stability of the complexes on storage at 4 °C, for up to a month, compared to a slow doubling in size of non-cholesterol-containing nanocomplexes. This may be due to the increased rigidity of the membranes with incorporated cholesterol, making the nanocomplexes resistant to aggregation or to degradation.
It was also found that the intensity of fluorescence reduced over time with cholesterol-containing formulations, probably due to higher escape from endosomes and thus their ability to diffuse through the cytosol.
Transfection of the potentially useful immunotherapeutic agent interleukin 15 (IL-15) was more than doubled with the optimized formulation. Further studies are planned to explore how this formulation affects the delivery of IL-15 by intra-tumor and intravenous delivery, perhaps with required modifications.
Implications
The study indicates the great potential for an optimized delivery system for mRNA, using nanocomplex principles but developed along different lines to account for the differences in biochemistry and biophysics of this molecule compared to other forms of RNA or DNA.
Simple steps such as the addition of cholesterol, the order of addition of the peptide, and introducing a different peptide with appropriate receptor-targeting and furin cleavage site characteristics, led to significant improvement in the efficiency of transfection. This indicates the benefits of the multifactorial approach to optimization, identifying the critical sites for alteration.
Read the original article on News Medical.