In cancer research, it has been increasingly known that tumour cells can change the alliance of some specific macrophages to help the tumour grow. “Macrophages are cells that act like the vacuum cleaners of your immune system. Normally they catch intruders and destroy them, but tumour cells can hijack these cells to help them spread throughout the body,” Prakash explains.
Tail-flipping nanoparticles
Prakash and his team designed nanoparticles that train these tumour-supporting ‘bad’ macrophages into cells that will fight tumours. However, these tiny (100-200 nanometre diameter) cell-like structures first have to find the macrophages before they can start the training. Prakash says: “It was one of the questions we tried to answer with this research: How do we get our nanoparticles at the right location and to the right macrophage.”
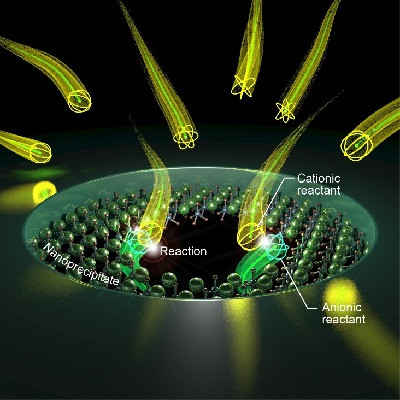
To solve this challenge, the researchers had to alter the nanoparticles. The nanoparticles consist of a double layer of specific lipids (phospholipids) called nanoliposomes. These lipids have long tails that like to stick together in between the double layer. “We replaced some of the lipids to ones with a slightly shorter charged tail that can ‘flip’ to the outer surface,” Prakash explains. The bad macrophages can recognize these flipped tails and then eat up the whole particle.
Training macrophages
“When we knew how to target the bad macrophages, it became time to train them into fighting the tumour again”, Prakash says. The researchers added a small component of the bacterial cell wall, which can train macrophages, to the ‘tail-flipping’ nanoliposomes in the double layer wall of these nanoparticles. These molecules are then also taken up by the bad macrophages which subsequently train them to kill cancer cells. Targeting this compound this way prevents it from being recognized by the wrong cells and thus prevents damage to other parts of the body.
Killing tumours and preventing metastasis
In the publication, the researchers not only show that the hijacked macrophages can be retrained to fight the cancer cells again, inhibiting the tumour growth by 70% in breast tumour mouse models. “In our mice, the therapy prevented metastasis, the ability of cancer cells to spread through the body,” Prakash says. The trained macrophages prevented the tumour cells from ‘preparing’ lung tissue to host tumour cells – a process before metastasis. When a tumour cell arrived in the lungs, the tissue wasn’t ready and the tumour cell couldn’t start a new tumour.
Read the original article on University of Twente (UT).