Although chemotherapy can be a lifesaving treatment for patients with cancer, some of these medications can damage the heart. A team led by researchers at Massachusetts General Hospital (MGH) recently developed a nanoparticle probe that can detect an indicator of heart damage from chemotherapy.
Experiments with the probe also revealed that in mice with cancer, intermittent fasting before chemotherapy can prevent this heart damage indicator from arising, leading to preserved cardiac function and prolonged survival.
The study, which is published in Nature Biomedical Engineering, focused on autophagy—a process that cells use to remove unnecessary or dysfunctional components. A delicate balance exists between the protective and deleterious effects of this process: reduced levels of autophagy have been implicated in cardiovascular disease and other conditions; however, autophagy can also be a primary mechanism of cell death.
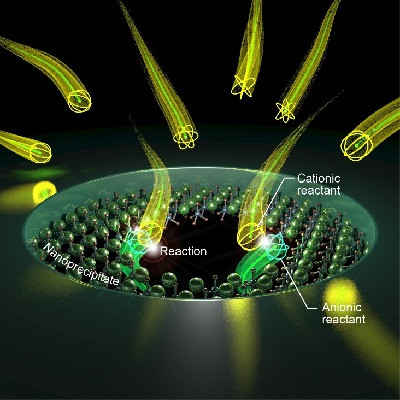
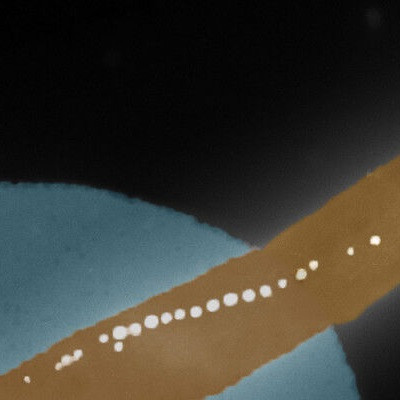
David E. Sosnovik, MD, director of the Program in Cardiovascular Imaging at MGH’s Martinos Center for Biomedical Imaging, and his colleagues developed an autophagy-detecting nanoparticle that allows investigators to measure autophagy’s activity non-invasively within the body, through either fluorescent or magnetic resonance imaging.
When the scientists intravenously injected the nanoparticles into mice with cancer, they could measure changes in autophagy in heart tissue under different conditions, such as after chemotherapy. For example, the nanoparticles detected reduced autophagy activity in heart cells exposed to the chemotherapy drug doxorubicin, which can cause heart damage. However, treatment with statins or fasting before doxorubicin treatment allowed the animals’ heart cells to maintain normal autophagy activity.
“We show with our nanoparticle that intermittent fasting—drinking water but no food for 24 hours before the chemotherapy is given—restores autophagy, eliminates the damage to the heart muscle, and even improves overall survival,” says Sosnovik, the senior author of the study.
Sosnovik stresses that complementary research in humans is needed, especially since the effects of fasting on autophagy in a tumor are unclear. “We are not suggesting that patients today fast before their chemotherapy. This is something that will need to be studied further in controlled and vigorous clinical trials,” he says. “However, our paper provides important insights that may affect clinical care in the near future.”
Also, the team’s autophagy-detecting nanoparticles could be used to gain a better understanding of the role of autophagy in a broad range of diseases.
Funding for the study was provided by the National Institutes of Health.
Read the original article on Massachusetts General Hospital.