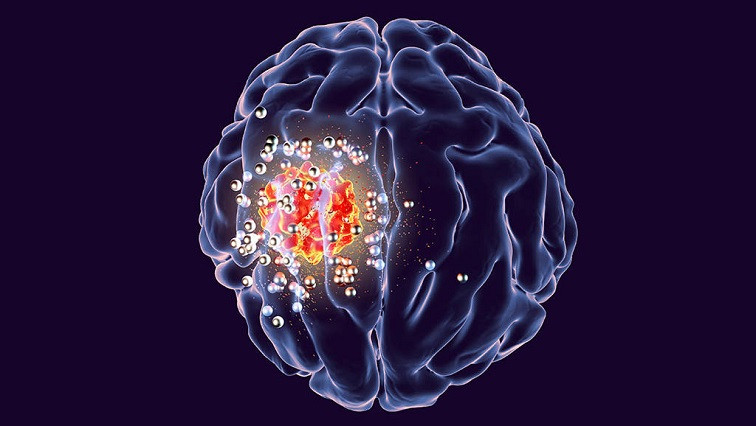
Brain tumors are among the most deadly and difficult-to-treat cancers. Glioblastoma, a particularly aggressive form, kills more than 10,000 Americans a year and has a median survival time of less than 15 months.
For patients with brain tumors, treatment typically includes open-skull surgery to remove as much of the tumor as possible followed by chemotherapy or radiation, which come with serious side effects and numerous hospital visits.
What if a patient's brain tumor could be treated painlessly, without anesthesia, in the comfort of their home? Researchers at Stanford Medicine have developed, and tested in mice, a small wireless device that one day could do just that. The device is a remotely activated implant that can heat up nanoparticles injected into the tumor, gradually killing cancerous cells.
In mice with brain tumors, 15 minutes of daily treatment over 15 days, as the animals went about their normal activities, was enough to significantly increase survival times. The researchers published their work in August in Nature Nanotechnology.
"The nanoparticles help us target the treatment to only the tumor, so the side effects will be relatively less compared with chemotherapy and radiation," said Hamed Arami, PhD, co-lead author of the paper, a former postdoctoral fellow at Stanford Medicine who is now at Arizona State University.
Arami, trained as a bioengineer, came to focus on brain cancer as a postdoctoral fellow in the lab of the late Sam Gambhir, MD, former chair of radiology at Stanford Medicine and a pioneer in molecular imaging and cancer diagnostics who died of cancer in 2020 . Five years prior, Gambhir's teenage son, Milan, died of a glioblastoma.
"There was a real passion in his lab to fight against this type of cancer," Arami said.
Heat treatment
Photothermal treatment of brain tumors -- using light to heat up nanoparticles -- had been done before, but it could be performed only during surgery, when the brain tumor was exposed to the light source.
Hoping to develop a system that did not require baring the brain, Gambhir had reached out to Ada Poon, PhD, a Stanford University associate professor of electrical engineering, who specializes in wireless devices that can integrate with the body.
"When I got that email from Sam, I saw that what he wanted to do was really aligned with what our lab is focusing on, which is using electronics to treat diseases," said Poon, who shares senior authorship with Gambhir.
Over a four-year collaboration, the team created a system that can generate heat precisely at the site of tumors to kill them. A small, wirelessly powered device is implanted between the skin and the skull. Then specially designed gold nanoparticles are injected into the tumor through a tiny hole in the skull.
When turned on, the device emits infrared light that can penetrate brain tissue to activate the nanoparticles, which increase in temperature by up to 5 degrees Celsius. That's enough to kill the cancer cells over repeated treatments without damaging the surrounding brain tissue.
By adjusting the power and wavelength of light, researchers can target tumors of different sizes and locations in the brain. The structure and dosage of the nanoparticles are calibrated to generate just the right amount of heat.
The researchers tested their device in mice that had been given human-derived brain tumors. The mice appeared to be undisturbed.
"We think this short amount of heating, which is in the clinically acceptable range, is not affecting normal activities," Arami said.
The researchers also showed that the injected nanoparticles stayed at the tumor site and did not endanger surrounding tissues.
Extending life
The treated mice lived significantly longer than the untreated mice, with doubled or tripled survival times on average, though the researchers caution that it's difficult to extrapolate survival benefit across species with such different lifespans. When the new treatment was combined with chemotherapy, the mice lived even longer.
"Glioblastoma patients don't often live more than two to three years after diagnosis because you can't get rid of every part of the tumor, and the tumor can become drug-resistant or radiation-resistant," Arami said. "The goal is to combine this with other treatments to extend survival."
The researchers envision that their device, when adapted to human patients, could be used for in-home treatment in addition to surgery, chemotherapy or radiation, without adding to the burden of hospital visits or interrupting their normal lives.
The researchers are confident they can scale up the device for human-sized brains. "With the rapid progress in the field of device development, I think that, in the next five years, we'll be able to develop devices that can generate even more optical powers for deeper tumors," Arami said.
"Actually," Poon added, "a lot of the challenge from the engineering side was how to make the devices small enough to fit the mouse brain."
Read the original article on Stanford Medicine.